Moles
Nevi or moles are common benign skin growths. Typically, they are either flat or slightly raised pigmented or skin colored lesions. Age, race, genetic and environmental factors (primarily sun exposure) all contribute to the development of nevi. They can develop anywhere on the body and usually appear within the early adult years. Most nevi are categorized by histologic subtypes such as the junctional, compound, or intradermal being the more common.
While most are considered benign, some nevi may be atypical or dysplastic and need to be distinguished from melanoma. Signs of worrisome atypia include Asymmetry, irregular Border, uneven or multiple Colors, large Diameter (>6 mm) and Evolution or changing. These features constitute the ABCDEs of melanoma. Regular self examinations are important. If such features are present, a focused skin evaluation is warranted and a biopsy may be necessary. Persons with many atypical moles or with a family history of melanoma are at a higher risk and need regular medical screening and evaluation.
Being born with large moles are called congenital nevi. On an infant, such moles are classified as large if they're more than 2 inches (5 centimeters) in diameter. Even a large mole seldom becomes cancerous and almost never before the child reaches puberty.
This mole often looks like melanoma. It can so closely resemble melanoma that a dermatologist cannot tell by looking at it. That’s because this mole is often is pink, raised, and dome-shaped. It also can have different colors in it such as red, black, and brown. The mole may bleed and it can have an opening that oozes.
When a mole appears on the skin after a person is born, it is called an acquired mole. Most people who have light skin have about 10 to 40 of these moles. These moles also are called common moles.If a person has 50 or more of these moles, the person has a higher risk for getting melanoma.
The majority of skin lesions are benign and are commonly seen. Many can be safely observed while others may require treatment of surgical intervention. When a new lesion or mark appears on your skin it can be difficult to tell whether it is benign or malignant. If you have any suspicions or concerns about a mark, mole or lesion you should get it checked immediately. The following is a list of some commonly seen and treated benign lesions at Carolinas Skin Center.

Examine both halves of the lesion to determine symmetry. One half appearing different than the other side may be concerning.

Look at the border around the lesion. Determine if there is an irregular, scalloped or poorly defined outline.

Visualize and compare the colors throughout the lesion. Multiple shades and scattered variations may be worrisome.

Gauge and measure the diameter of the lesion. Melanomas are usually greater than 6mm (the size of a pencil eraser) when diagnosed, but they can be smaller in size.

Consider how the lesion looked previously or how it compares to other areas. A mole that changes in size, shape or color or looks different than others should be medically examined.
When should I seek medical assistance?
If you notice any changes in your moles that fit the ABCDE criteria or if you have concerns about a new or existing mole, it's advisable to consult with a healthcare professional. Regular skin checks and prompt evaluation of any suspicious moles are crucial for early detection and treatment of skin cancer. In some cases, a biopsy may be performed to rule out any potential concerns, such as melanoma.
Regular self-examinations and professional skin checks are particularly important if you or anyone in your family has had a melanoma.
Sometimes suspicious moles may need to be biopsied or simply removed if they are bothersome or being traumatized and irritated because of their location.
Schedule Your Appointment Now


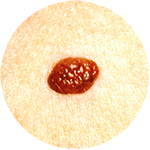 Cherry Angioma
Cherry Angioma 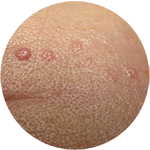 Sebaceous Hyperplasia (Senile Hyperplasia)
Sebaceous Hyperplasia (Senile Hyperplasia)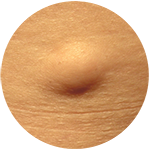 Lipoma
Lipoma Seborrheic Keratosis
Seborrheic Keratosis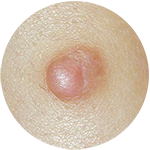 Dermatofibroma
Dermatofibroma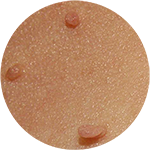 Acrochordon
Acrochordon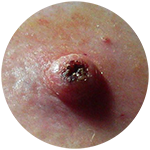 Keratoacanthoma
Keratoacanthoma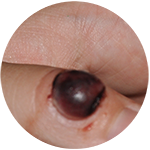 Pyogenic Granuloma
Pyogenic Granuloma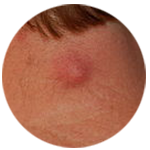 Epidermoid Cyst
Epidermoid Cyst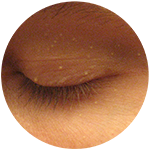 Milia
Milia